The following is based on information provided by the National Organization for Albinism and Hypopigmentation (NOAH). At times, the information is highly technical and contains specialized language. This is also the case with the text of the National Health Service (NHS, UK). More common language is being used by the international news agency, ALJAZEERA, and by – of course – Wikipedia.
National Organization for Albinism and Hypopigmentation (NOAH)
Albinism is an inherited genetic condition that reduces the amount of melanin pigment formed in the skin, hair and/or eyes. Albinism occurs in all racial and ethnic groups throughout the world. In the U.S., approximately one in 18,000 to 20,000 people has some type of albinism. In other parts of the world, the occurrence can be as high as one in 3,000. Most children with albinism are born to parents whose hair and eye color are typical for their ethnic backgrounds.
A common myth is that people with albinism have red eyes. Although lighting conditions can allow the blood vessels at the back of the eye to be seen, which can cause the eyes to look reddish or violet, most people with albinism have blue eyes, and some have hazel or brown eyes. There are different types of albinism and the amount of pigment in the eyes varies. However, vision problems are associated with albinism.
Vision Considerations
People with albinism have vision problems that are not correctable with eyeglasses, and many have low vision. It’s the abnormal development of the retina and abnormal patterns of nerve connections between the eye and the brain that cause vision problems. The presence of these eye problems defines the diagnosis of albinism.
The degree of impairment varies with the different types of albinism. Although people with albinism may be considered “legally blind” with a corrected visual acuity of 20/200 or worse, most learn to use their vision in a variety of ways and are able to perform innumerable activities such as reading, riding a bike or fishing. Some have sufficient vision to drive a car.
Dermatological Considerations
Because most people with albinism have fair complexions, it’s important to avoid sun damage to the skin and eyes by taking precautions such as wearing sunscreen or sunblock, hats, sunglasses and sun-protective clothing.
Types of Albinism
While most people with albinism have very light skin and hair, levels of pigmentation can vary depending on one’s type of albinism. Oculocutaneous (pronounced ock-you-low-kew-TAIN-ee-us) albinism (OCA) involves the eyes, hair and skin.
Ocular albinism (OA), which is much less common, involves only the eyes, while skin and hair may appear similar or slightly lighter than that of other family members.
Over the years, researchers have used various systems for classifying oculocutaneous albinism. In general, these systems contrasted types of albinism having almost no pigmentation with types having slight pigmentation. In less pigmented types of albinism, hair and skin are cream-colored and vision is often in the range of 20/200. In types with slight pigmentation, hair appears more yellow or has a reddish tinge and vision may be better.
DNA tests can determine the precise type of albinism. Research on albinism genes is ongoing. To date as many as seven forms of oculocutaneous albinism are now recognized – OCA1, OCA2, OCA3, OCA4, OCA5, OCA6 and OCA7. Some are further divided into subtypes.
• OCA1, or tyrosinase-related albinism, results from a genetic defect in an enzyme called tyrosinase. This enzyme helps the body to change the amino acid, tyrosine, into pigment. (An amino acid is a “building block” of protein.) There are two subtypes of OCA1. In OCA1A, the enzyme is inactive and no melanin is produced, leading to white hair and very light skin. In OCA1B, the enzyme is minimally active and a small amount of melanin is produced, leading to hair that may darken to blond, yellow/orange or even light brown, as well as slightly more pigment in the skin.
• OCA2, or P gene albinism, results from a genetic defect in the P protein that helps the tyrosinase enzyme to function. People with OCA2 make a minimal amount of melanin pigment and can have hair color ranging from very light blond to brown.
• OCA3 is rarely described and results from a genetic defect in TYRP1, a protein related to tyrosinase. People with OCA3 can have substantial pigment.
• OCA4 results from a genetic defect in the SLC45A2 protein that helps the tyrosinase enzyme to function. People with OCA4 make a minimal amount of melanin pigment similar to people with OCA2.
• OCA5–7 were recognized in humans in 2012 and 2013. They have reported mutations on three additional causative genes. As gene testing becomes available, and more people with these types of albinism are identified, the complete range of physical manifestations will be recognized, and may overlap with other known types of OCA. Currently, these types of albinism are considered to be uncommon.
Researchers have also identified several other genes that result in albinism with other features. One group includes at least 10 genes leading to Hermansky-Pudlak Syndrome (HPS). In addition to albinism, HPS is associated with bleeding problems and bruising. Some forms are also associated with lung and bowel disease. HPS is a less common form of albinism but should be suspected if a person with albinism shows unusual bruising or bleeding or if a genetic test for a type of OCA produces inconclusive results.
Other albinism-related syndromes include Chediak-Higashi Syndrome and Griscelli Syndrome.
Genetics of Albinism
The genes for OCA are located on “autosomal” chromosomes. Autosomes are the 22 pairs of chromosomes that contain genes for our general body characteristics, compared to the one pair of sex chromosomes. We normally have two copies of these chromosomes and the many genes on them – one inherited from our father, the other inherited from our mother. For a recessive trait (like most types of albinism) to occur, both of the person’s chromosomes must carry that trait. That means that most types of albinism result from inheriting an albinism trait from both the mother and the father who often have typical pigmentation. In this case, the mother and father are considered to be carriers of the albinism trait because they each carry a recessive gene for the condition but do not manifest the condition themselves. When both parents carry the albinism gene (and neither parent has albinism) there is a one in four chance at each pregnancy that the baby will be born with albinism. This type of inheritance is called “autosomal recessive” inheritance.
Ocular albinism (OA1) is caused by a change in the GPR143 gene that plays a signaling role that is especially important to pigmentation in the eye. OA1 follows a simpler pattern of inheritance because the gene for OA1 is on the X chromosome. Females have two copies of the X chromosome while males have only one copy (and a Y chromosome that makes them male). To have ocular albinism, a male only needs to inherit one changed copy of the gene for ocular albinism from his carrier mother. Therefore almost all of the people with OA1 are males. Parents should be suspicious if a female child is said to have ocular albinism. While possible if the mother is a carrier of ocular albinism and the father has ocular albinism, it is extremely rare.
For couples who have not had a child with albinism, there is no simple test to determine whether a person carries a gene for albinism. Researchers have analyzed the DNA of many people with albinism and found the changes that cause albinism, but these changes are not always in exactly the same place, even for a given type of albinism. Moreover, many of the tests do not find all possible changes. Therefore, the tests for the albinism gene may be inconclusive. If parents have had a child with albinism previously, and if that affected child has had a confirmed diagnosis by DNA analysis, there is a way to test in subsequent pregnancies to see if the fetus has albinism. The test uses either amniocentesis (placing a needle into the uterus to draw off fluid) or chorionic villous sampling (CVS). Cells in the fluid are examined to see if they have an albinism gene from each parent.
For specific information and genetic testing, seek the advice of a qualified geneticist or genetic counselor. The American College of Medical Genetics and the National Society of Genetic Counselors maintain a referral list. Those considering prenatal testing should be made aware that people with albinism usually adapt quite well to their disabilities and lead very fulfilling lives.
Vision Rehabilitation
Eye problems in albinism result from the abnormal development of the eye because of a lack of pigment and often include:
• Nystagmus: Regular horizontal back and forth movement of the eyes
• Strabismus: Muscle imbalance of the eyes, “crossed eyes” (esotropia), “lazy eye” or an eye that deviates out (exotropia)
• Photophobia: Sensitivity to bright light and glare
• Refractive Error: People with albinism may be either farsighted or nearsighted and usually have astigmatism
• Foveal hypoplasia: The retina, the surface inside the eye that receives light, does not develop normally before birth and in infancy
• Optic nerve misrouting: The nerve signals from the retina to the brain do not follow the usual nerve routes
The iris, the colored area in the center of the eye, has very little or no pigment to screen out stray light coming into the eye. Light normally enters the eye only through the pupil, the dark opening in the center of the iris, but in albinism light can pass through the iris as well.
For the most part, treatment consists of visual rehabilitation. Surgery to correct strabismus may improve the appearance of the eyes. However, since surgery will not correct the misrouting of nerves from the eyes to the brain, surgery will not improve eyesight or fine binocular vision. In the case of esotropia or “crossed eyes,” surgery may help vision by expanding the visual field (the area that the eyes can see while looking at one point). Surgical intervention is also available to minimize nystagmus.
People with albinism are sensitive to glare, but they do not prefer to be in the dark, and they need light to see just like anyone else. Sunglasses or tinted contact lenses may help outdoors. Indoors, it is important to place lights for reading or close work over a shoulder rather than in front.
Various optical aids are helpful to people with albinism, and the choice of an optical aid depends on how a person uses his or her eyes in jobs, hobbies or other usual activities. Some people do well using bifocals which have a strong reading lens, prescription reading glasses or contact lenses. Others use handheld magnifiers or special small telescopes, and some prefer to use screen magnification products on computers.
Some people with albinism use bioptics, glasses which have small telescopes mounted on, in or behind their regular lenses so that one can look through either the regular lens or the telescope. Some states allow the use of bioptic telescopes for driving.
Optometrists or ophthalmologists who are experienced in working with low vision patients can recommend various optical aids. Clinics should provide instruction in their use. The American Foundation for the Blind maintains a directory of low vision clinics. In Canada, support is available from the Canadian National Institute for the Blind.
Medical Problems
In the United States, most people with albinism live normal life spans and have the same types of general medical problems as the rest of the population. The lives of people with Hermansky-Pudlak Syndrome can be shortened by lung disease or other medical problems.
In tropical countries, people with albinism who do not have access to adequate skin protection may develop life-threatening skin cancers. If they use appropriate skin protection, such as sunscreens rated 20 SPF or higher and opaque clothing, people with albinism can enjoy outdoor activities even in summer.
Social Considerations
People with albinism are at risk of isolation because the condition is often misunderstood. Social stigmatization can occur, especially within communities of color, where the race or paternity of a person with albinism may be questioned. Families and schools must make an effort to include children with albinism in group activities. Contact with others with albinism or who have albinism in their families or communities is most helpful. NOAH can provide the names of contacts in many regions of the country.
Source: National Organization for Albinism and Hypopigmentation (NOAH): Information Bulletin

ALJAZEERA
Albinism occurs globally, in all genders, racial and ethnic groups. Although in Europe and North America approximately 1 in 20,000 people have albinism, the rates are higher in Africa with an estimated 1 in 5,000 likely to have albinism in Tanzania.
Albinism is a lifelong condition and does not cause intellectual disabilities. However, the poor health and poor vision of people with albinism often results in some abandoning school.
Historically, the term “albino” has been used in a derogatory manner, so “person with albinism” is preferred when referring to people with albinism.
Why are there so many people with albinism in Africa? Is albinism limited to a race group?
What is albinism?
Albinism is a congenital disorder that results in a lack of pigmentation (known as melanin) that gives colour to hair, skin and eyes. Other conditions associated with albinism include vulnerability to bright light, which can cause legal blindness.
Because their skin is particularly vulnerable to the sun’s ultraviolet rays, people with albinism can also be predisposed to skin cancer and lesions. According to a 2014 study, people with albinism in Africa are 1,000 times more likely to get skin cancer than others.
There are five genetic types of albinism, the most common being oculocutaneous (“oculo” meaning eye and “cutaneous” meaning skin) type 1 (OCA1) and type 2 (OCA2).
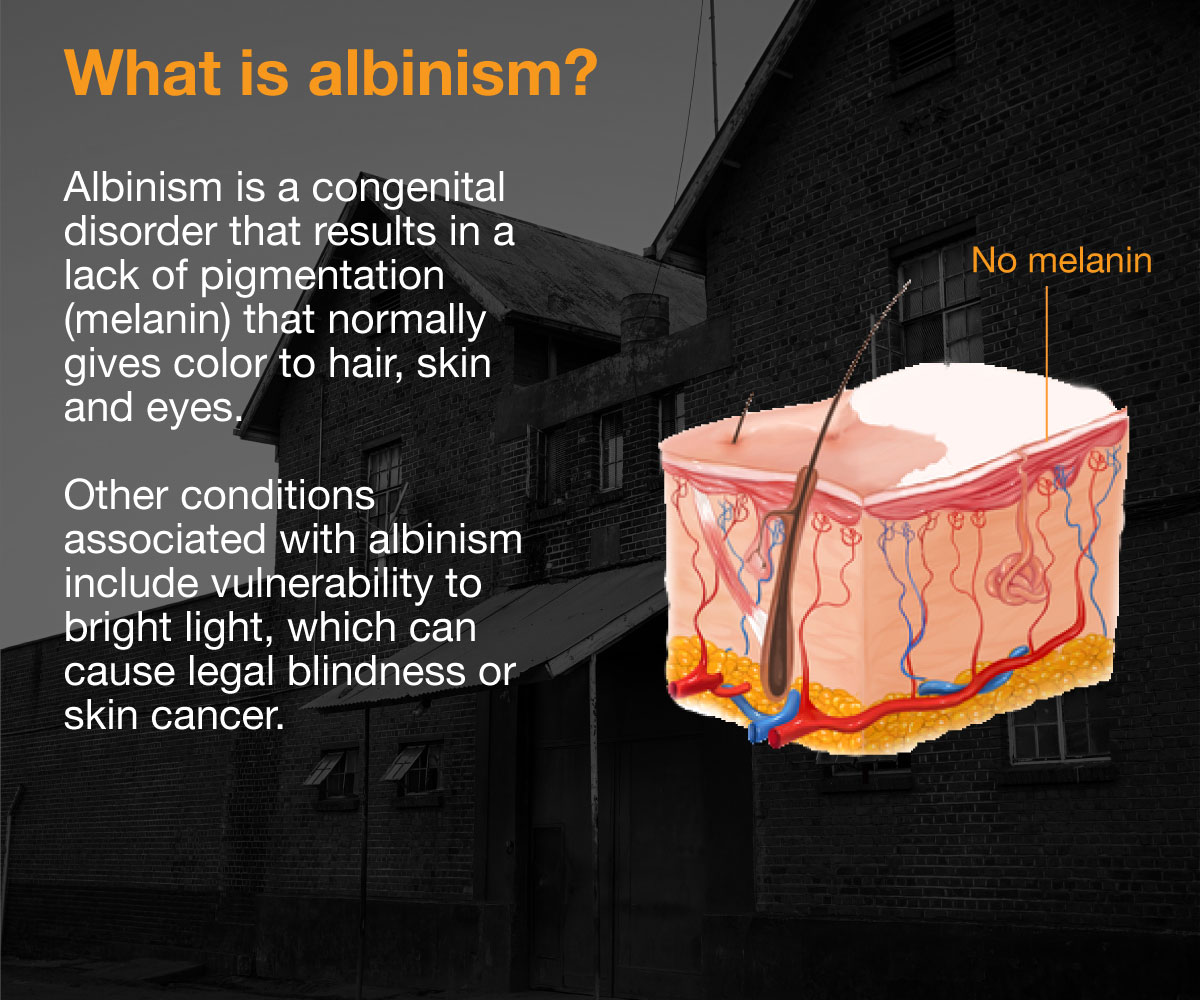 |
What causes albinism?
Albinism is caused by a recessive gene, meaning both parents must carry the gene for it to be passed on. The parents themselves do not need to exhibit albinism.
Many children with albinism have blue or brown eyes. Sometimes, the eyes might appear pink or reddish, and that is a result of the iris having very little colour. Albinism is a lifelong condition and does not cause intellectual disabilities.
Children with albinism usually have normal intelligence but their poor health and poor vision can often result in persons with albinism abandoning schooling.
People with albinism are considered legally blind because their photoreceptors (or cells in the retina that detect light) are unable to adequately convert light into clear signals to the brain. As a result, persons with albinism have a condition called nystagmus. This is when the eyes continuously flutter. They may also have problems with reduced depth perception and with tracking an object with their eyes.

How common is albinism?
Albinism occurs globally, in all gender, racial and ethnic groups. Estimates of affected people as part of the general population vary from region to region. The highest rate is in Sub-Saharan Africa with an estimated 1 in 5,000 people likely to be a person with albinism in Tanzania.
What is the preferred term?
The term “albino” has historically been used in a derogatory manner, so “person with albinism” is preferred when referring to people with albinism. “Albino” also defines a person by his appearance, but “person with albinism” puts the person before their condition.

What are some myths about people with albinism?








Source: ALJAZEERA, What is albinism and what causes it?
National Health Service (NHS), UK
Albinism affects the production of melanin, the pigment that colours skin, hair and eyes. It’s a lifelong condition, but it does not get worse over time.
People with albinism have a reduced amount of melanin, or no melanin at all. This can affect their colouring and their eyesight.
People with albinism often have white or very light blonde hair, although some have brown or ginger hair. The exact colour depends on how much melanin their body produces.
Very pale skin that burns easily in the sun and does not usually tan is also typical of albinism.
Eye problems
The reduced amount of melanin can cause eye problems. This is because melanin is involved in the development of the retina, the thin layer of cells at the back of the eye.
Possible eye problems linked to albinism include:
- poor eyesight – either short-sightedness or long-sightedness, and low vision (sight loss that cannot be corrected)
- astigmatism – where the cornea (clear layer at the front of the eye) is not perfectly curved or the lens is an abnormal shape, causing blurred vision
- photophobia – where the eyes are sensitive to light
- nystagmus – where the eyes move involuntarily from side to side, causing reduced vision; you do not see the world as “wobbling” because your brain adapts to your eye movement
- squint – where the eyes point in different directions
Some young children with albinism may appear clumsy. This is because problems with their eyesight can make some movements difficult for them, such as picking up an object. This should improve as they get older.
How albinism is passed on
The 2 main types of albinism are:
- oculocutaneous albinism (OCA) – the most common type, affecting the skin, hair and eyes
- ocular albinism (OA) – a rarer type that mainly affects the eyes
Autosomal recessive inheritance
In all types of OCA and some types of OA, albinism is passed on in an autosomal recessive inheritance pattern. This means a child has to get 2 copies of the gene that causes albinism (1 from each parent) to have the condition.
If both parents carry the gene, there’s a 1 in 4 chance that their child will have albinism and a 1 in 2 chance that their child will be a carrier. Carriers do not have albinism but can pass on the gene.
X-linked inheritance
Some types of OA are passed on in an X-linked inheritance pattern. This pattern affects boys and girls differently: girls who get the albinism gene become carriers, while boys who get it will have albinism.
When a mother is a carrier of an X-linked type of albinism, each of her daughters has a 1 in 2 chance of becoming a carrier. Each of her sons has a 1 in 2 chance of having albinism.
When a father has an X-linked type of albinism, his daughters will become carriers, and his sons will not have albinism and will not be carriers.
Genetic counselling
If you have a history of albinism in your family or you have a child with the condition, you may want to talk to a GP about getting a referral for genetic counselling.
A genetic counsellor provides information, support and advice about genetic conditions. For example, you can discuss with them how you inherited albinism and the chances of passing it on.
Read more about genetic testing and counselling
Diagnosing albinism
Albinism is usually obvious from a baby’s appearance when they’re born. Your baby’s hair, skin and eyes may be examined to look for signs of missing pigment.
As albinism can cause a number of eye problems, your baby may be referred to an eye specialist (ophthalmologist) for tests.
Electrodiagnostic testing is also sometimes used to help diagnose albinism. This is where small electrodes are stuck to the scalp to test the connections of the eyes to the part of the brain that controls vision.
Treatments for eye problems due to albinism
Although there’s no cure for the eye problems caused by albinism, there are a number of treatments, such as glasses and contact lenses, that can improve vision.
A child with albinism may also need extra help and support at school.
Glasses and contact lenses
As a child with albinism gets older, they’ll need regular eye tests, and it’s likely they’ll need to wear glasses or contact lenses to correct vision problems.
Low-vision aids
Vision aids include:
- large-print or high-contrast books and printed materials
- magnifying lenses
- a small telescope or telescopic lenses that attach to glasses to read writing in the distance, such as on a school whiteboard
- large computer screens
- software that can turn speech into typing or vice versa
- tablets and phones that allow you to magnify the display to make writing and images easier to see
The Royal National Institute of Blind People (RNIB) has more information about living with low vision, including a section on education and learning.
Photophobia or sensitivity to light
Sunglasses, tinted glasses and wearing a wide-brimmed hat outside can help with sensitivity to light.
Nystagmus
There’s currently no cure for nystagmus (where the eyes move from side to side involuntarily). However, it is not painful and does not get worse.
Certain toys or games may help a child make the most of the vision they have. An ophthalmologist will be able to provide further advice.
Surgery, involving dividing and then reattaching some of the eye muscles, may sometimes be an option.
Squint and lazy eye
The main treatments for squints are glasses, eye exercises, surgery and injections into the eye muscles.
If your child has developed a lazy eye, they may benefit from wearing a patch over their “good” eye to encourage their other eye to work harder.
Read more about treatments for squints
Reducing the risk of sunburn and skin cancer
Because people with albinism lack melanin in their skin, they’re at increased risk of getting sunburn and skin cancer.
If you have albinism, you should wear sunscreen with a high sun-protection factor (SPF). An SPF of 30 or more will provide the best protection.
It’s also a good idea to look out for skin changes, such as:
- a new mole, growth or lump
- any moles, freckles or patches of skin that change in size, shape or colour
Report these to a doctor as soon as possible. Skin cancer is much easier to treat if it’s found early.
Help and support
There’s usually no reason why someone with albinism cannot do well in normal schooling, further education and employment.
With appropriate help and support, most children with albinism can attend a mainstream school.
You might like to talk to other people with albinism. The Albinism Fellowship has a contact person network that can provide advice and support locally.
Information about you
If you or your child has albinism, your clinical team will pass information on to the National Congenital Anomaly and Rare Disease Registration Service (NCARDRS).
The NCARDRS helps scientists look for better ways to prevent and treat this condition. You can opt out of the register at any time.
Source: National Health Service, UK
And, finally, Albinism in humans (Wikipedia)
